Despite a significant decrease in Sudden Infant Death Syndrome (SIDS), infant sleep-related mortality continues to affect many families in North Carolina. In North Carolina, SIDS and other sleep-related infant deaths are the leading cause of infant mortality in babies 1-12 months of age and the 3rd leading cause of death among all North Carolina infants. The majority of all of these deaths are associated with unsafe sleep environments.
Read below to learn more about SIDS and other sleep-related infant deaths and data trends specific to these deaths in North Carolina.
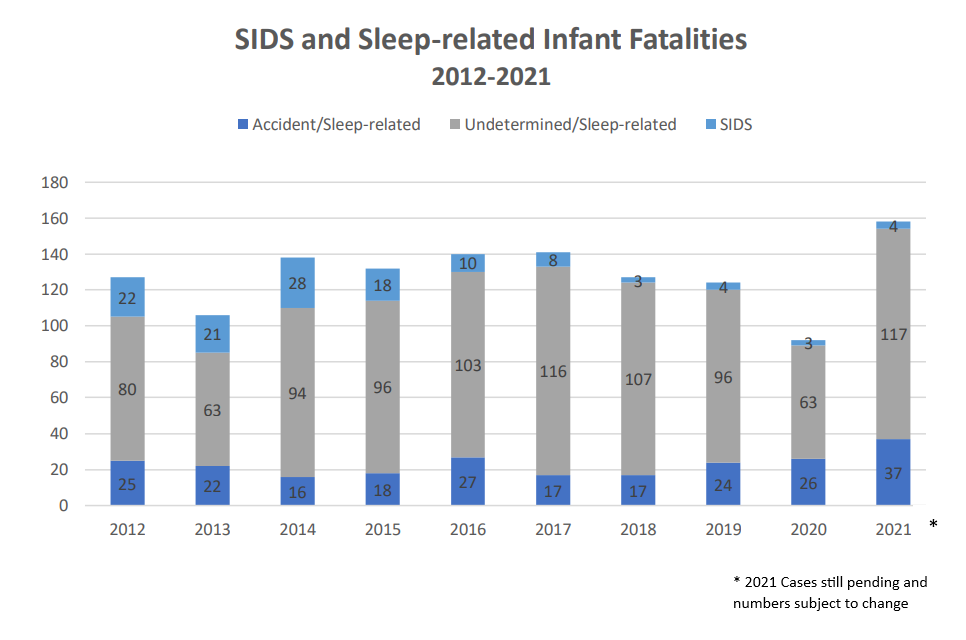
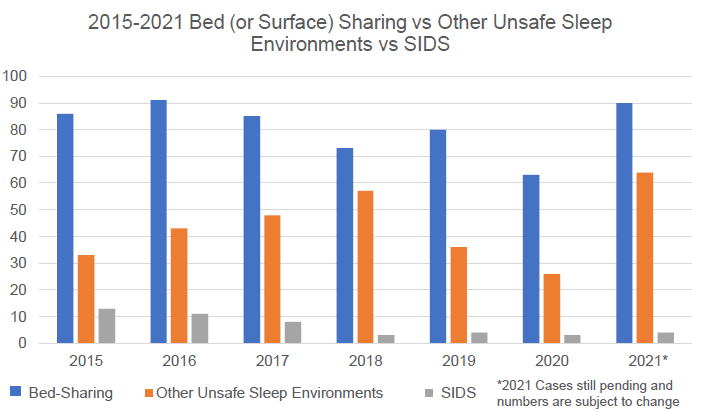
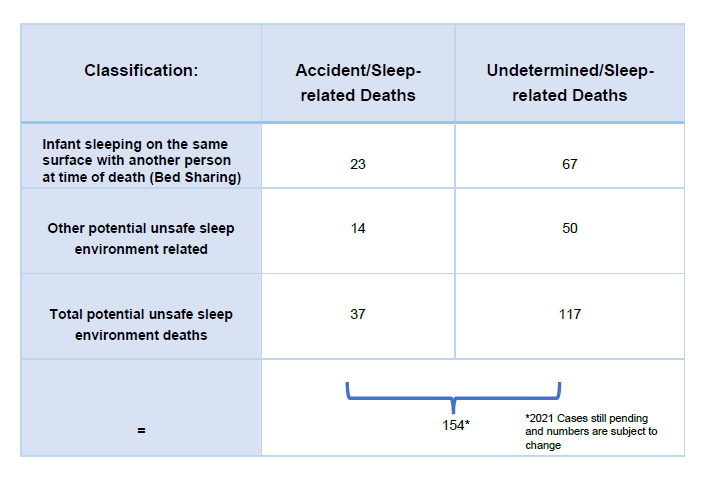
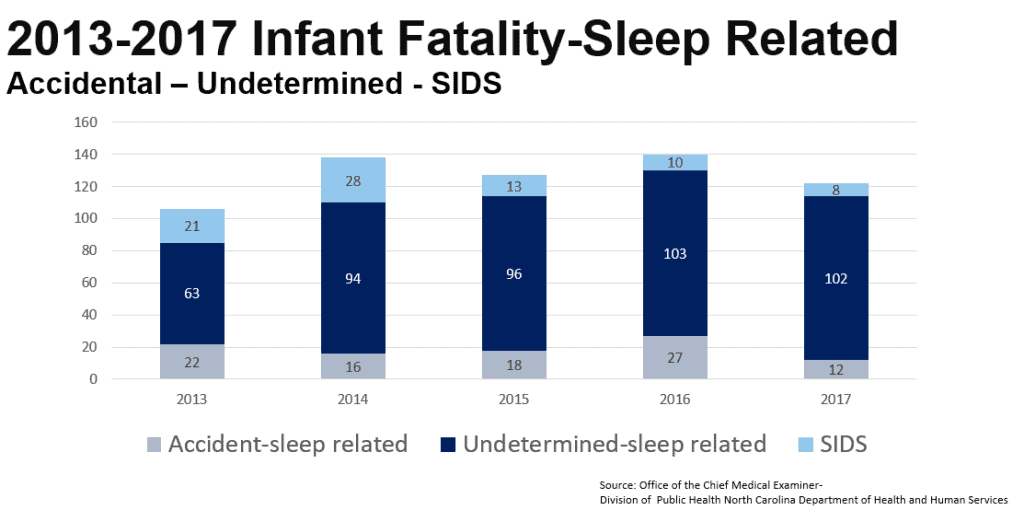
Sleep-related infant deaths are classified by the manner of death in three ways by the North Carolina Office of the Chief Medical Examiner: Accident, Undetermined, or Natural, which is when the death is classified as Sudden Infant Death Syndrome (SIDS). The large majority of deaths are associated with unsafe sleep environments. From 2013-2017, 641 of North Carolina infants died suddenly unexpectedly while sleeping. Of these deaths, 88% occurred in an unsafe sleep environment (for example, blankets in bed, sleeping on an adult bed, etc.). And 70% of these deaths were associated while bed sharing (when an individual is sleeping on the same surface with an infant).
SUID is the death of an infant younger than 1 year of age that occurs suddenly and unexpectedly.
After a full investigation, SUIDs that occur during an unobserved sleep period may be diagnosed as one of the three types of SUID:
- Natural: Sudden Infant Death Syndrome (SIDS)
- Accidental: Accidental suffocation and strangulation in bed (ASSB)
- Undetermined/Unknown
These investigations are often very complicated and this makes it difficult to make a diagnosis. This is why so many deaths are classified as undetermined and unknown.
Sudden Infant Death Syndrome (SIDS) is the sudden death of an infant younger than 1 year of age that cannot be explained even after a full investigation that includes a complete autopsy, examination of the death scene, and review of the clinical history. According to the Centers for Disease Control and Prevention, the overall rate of SIDS in the United States declined by more than 50% since 1990. However, better investigations of unexpected infant deaths and greater adoption of safe sleep practices may have contributed to fewer SIDS deaths.
Important to note: In North Carolina, if a sleep-related infant death was associated with an unsafe sleep environment, including bed sharing it would not be classified as SIDS.
Bed sharing is when an infant sleeps on the same surface (bed, couch, chair, etc.) as another person (parent, sibling, caregiver, etc.).
SIDS is…
- Nationally is the leading cause of death in infants between 1 month to 1 year of age.
- A sudden and silent medical disorder that can happen to a seemingly healthy infant.
- Currently unpredictable and unpreventable, but the risk can be reduced.
- A diagnosis of exclusion, in which the cause of death can be determined only after ruling out other causes.
- A recognized medical disorder listed in the International Classification of Diseases, 10th Revision (ICD-10).
- An infant death that leaves unanswered questions.
SIDS is NOT…
- The cause of every sudden infant death.
- The same as suffocation or caused by suffocation.
- Caused by vaccines, immunizations, or shots.
- Contagious.
- The result of neglect or child abuse.
- Caused by cribs.
- Caused by vomiting or choking.
- Preventable, but there are ways to reduce the risk.
What causes SIDS:
Researchers are not 100% sure what causes SIDS, but research evidence suggests that some infants who die of SIDS are born with brain abnormalities or defects. These abnormalities are typically found within a network of nerve cells that rely on the neurotransmitter serotonin. The cells are located in part of the brainstem that probably controls breathing, heart rate, blood pressure, temperature, and waking from sleep.
Scientists believe that brain defects alone may not be enough to cause a SIDS death. Evidence suggests that other events, such as not getting enough oxygen, getting too much carbon dioxide, overheating, or having an infection, must also occur for an infant to die from SIDS. Normally, infants sense this inadequate air intake, and their brains trigger them to wake up or trigger their heartbeat or breathing patterns to change or compensate. However, in a baby with abnormalities in the brainstem, these protective mechanisms may be missing or slower to occur, so the child may succumb to SIDS. Such a scenario might explain why babies who sleep on their stomachs are more susceptible to SIDS.
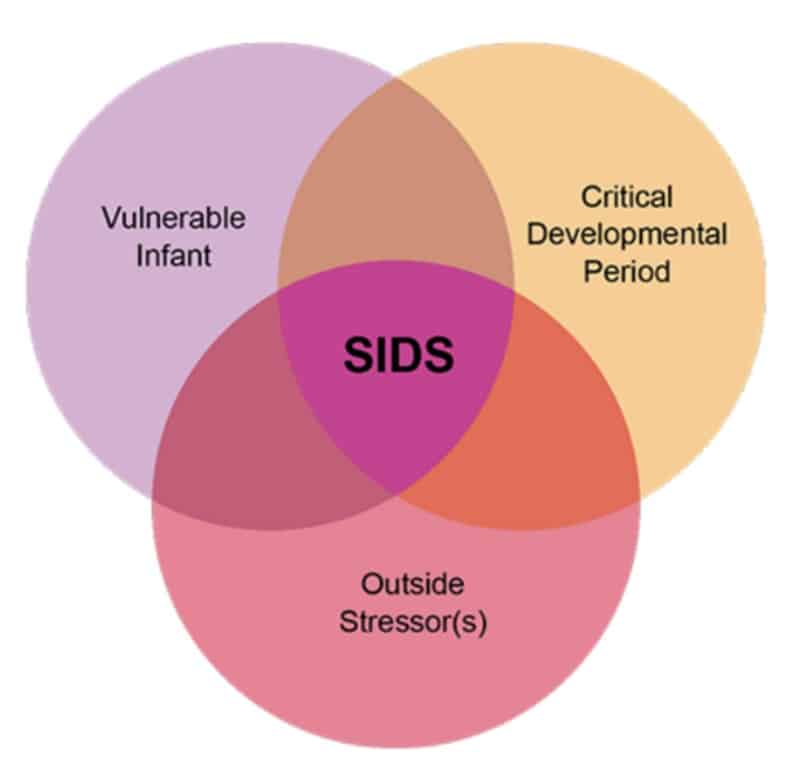
Researchers use the Triple-Risk Theory to explain this concept. According to the Triple-Risk Model, all three elements must be present for a sudden infant death to occur:
- The baby’s vulnerability is undetected.
- The infant is in a critical developmental period that can temporarily destabilize his or her systems.
- The infant is exposed to one or more outside stressors that he or she cannot overcome because of the first two factors.
Having only one of these features may not be enough to cause death from SIDS, but when all three combine, the likelihood of SIDS is high.
Risk factors that put infants at higher risk for SIDS
- Side and stomach (prone) sleep position
- Prenatal and postnatal tobacco smoke, alcohol, and illicit drug exposure
- Soft or cushioned sleep surfaces (including sofas, couches, armchairs)
- Bed sharing
- Soft bedding (including pillows, blankets, sheepskins, bumper pads, and positioners)
- Head covering and overheating
- Preterm or low birth weight infants
- Not being breastfed
Many of the risk factors for SIDS are strikingly similar to those of other sleep-related infant deaths.
Accidental Suffocation and Strangulation in Bed (ASSB): One type of SUID, ASSB is a cause-of-death code used for vital statistics purposes. This code is used to identify infant deaths caused by suffocation or asphyxia (blockage of the infant’s airway) in a sleeping environment. The classification of Accidental Suffocation and Strangulation in Bed is used by the Office of the Chief Medical Examiner when circumstances are definitively or strongly suggest the likelihood of asphyxiation.
These deaths are associated with unsafe sleeping environments for an infant. For example:
Suffocation by soft bedding: When soft bedding, a pillow, or a waterbed mattress blocks the infant’s airway.
Overlay: When another person shares the sleep surface with the infant and lays on or rolls on top of or against the infant while sleeping, blocking the infant’s airway.
Wedging or entrapment: When an infant gets trapped between two objects, such as a mattress and wall, bed frame, or furniture, blocking the infant’s airway.
Strangulation: When something presses on or wraps around the infant’s head and neck blocking the airway.
This classification is given when it is not certain why the infant died. Other manners or causes of death cannot be ruled out, so definite cause cannot be determined. The large majority of deaths fall into the Undetermined Classification.
Most sleep related infant deaths are associated with the infant sleeping in an unsafe sleep environment. It would be considered an unsafe sleep environment if the following was not practiced:
- Placing the baby on his or her back at all sleep times – including naps and at night.
- Using a firm sleep surface, such as a safety-approved mattress and crib.
- Keeping soft objects and loose bedding out of the baby’s sleep area.
- Sharing a room with baby, but not the same bed.